TMA resulting from inhibitors of vascular endothelial growth factors8,9 has been established to involve injury to renal podocytes. TMA resulting from quinine may involve immune injury to endothelial cells.10 Better understanding of the mechanisms of DITMA should provide a basis for better diagnosis and treatment. Failure to recognize a drug as the cause of TMA, especially immune-mediated TMA, may have critical consequences if the patient is reexposed to the drug. Drug-induced TMA (DiTMA) can be either dose- and time-dependent or non-dose-related (idiosyncratic reactions).
Gemcitabine

In health, the presence of several regulators of complement safeguards against inappropriate activation of C3b, but also allows for rapid complement activation when C3b is bound to a target, for example, during infection. This mechanism prevents uncontrolled activation of the complement system and attendant tissue injury. Other complement regulators increase the decay of convertases, the enzyme complexes necessary to drive complement activity.
2 Complement Inhibitor In DITMA Treatment
In fact, this is the most well-known mechanism for TKIs-induced TMA 62,67,69, 70, 71. The treatment of PDL-induced TMA relies on supportive care and drug withdrawal, most times resulting in TMA regression 56. Doxorubicin is an anthracycline that acts as a topoisomerase II inhibitor. Pegylated liposomal doxorubicin (PLD) is commonly used in recurrent ovarian cancer. This formulation markedly prolongs the half-life in the vascular compartment and limits its adverse effects 54,55. TMA is a well-recognized complication in Oncology setting, either as a consequence of cancer or of its treatments.
Serum creatinine levels will probably not provide a reliable estimation of GFR, because these patients may display large fluctuations in nutritional status, weight and muscle mass 91,97. Endothelial injury is also a feature of GVHD, with endothelial cells as the putative direct target of donor cytotoxic T lymphocytes 88,106,111. Patients with acute GVHD after HSCT present high levels of plasma markers of endothelial injury, indicating a probable link between endothelial lesion and the development of both GVHD and HSCT-TMA 8,106,112. Immunotherapy is an emerging strategy to treat solid and hematologic malignancies, improving overall survival.

4 Clinical Features And Laboratory Tests
Most patients had already been diagnosed with cancer, although it can occasionally be a presenting sign of malignancy 89,140. Unlike other paraneoplastic syndromes, there is a high number of cases of TiTMA that occur with cancer recurrence, probably due to changes in tumor cells properties as a consequence of chemotherapy 141. The difficulty of histologic diagnosis led to the development of non-invasive clinical criteria for HSCT-TMA diagnosis. The first ones were presented by the Bone Marrow Transplant Clinical Trials Network (BMT-CTN) 123 in 2005, followed by International Working Group (IWG) 124 in 2007. More recently, Jodele et al. 126 presented wider criteria that included kidney and/or neurological dysfunction. They define kidney manifestations as HTN, proteinuria ≥30 mg/dL or terminal complement activation.
Chemotherapy offers curative treatment for early stage cancer and palliation for late-stage cancer but may have off-target effects including kidney toxicity. One such adverse effect is TMA which constitutes microangiopathic hemolytic anemia (MAHA), thrombocytopenia, intravascular thrombosis, and ischemia-induced end-organ damage. This disease, now known as thrombotic thrombocytopenic purpura (TTP), is one of the most extensively studied subtypes of TMA. Primary TMAs mainly include hereditary or acquired forms of TTP and primary atypical hemolytic uremic syndrome (aHUS). Their pathogeneses are well-understood, and their respective diagnosis and treatment are well-developed. Drugs (including chemotherapy), pregnancy, malignant hypertension, autoimmune rheumatic diseases, infection, transplant, and malignancy constitute the secondary TMAs (Figure 1).
Advancing Acute Pain Care: Breakthrough Non-Opioid Therapies And The Pharmacist’s Critical Role
Direct injury to endothelial cells makes them more susceptible to TMA after another insult 147. On the other hand, indirect mechanisms rely on inhibiting proteins that regulate thrombosis, such as ADAMTS13, VWF, platelet membrane glycoprotein 1b and complement factor H. When the target is complement factor H, the paraprotein overactivates the alternative complement pathway, leading to C3 glomerulopathy or aHUS 147, 148, 149. Several studies evaluated plasmapheresis efficacy in this setting, with controversial evidence.
Drug-induced Thrombotic Microangiopathy: An Updated Review Of Causative Drugs, Pathophysiology, And Management
On the Self team, alternative pathway complement activation is the “offense”, alternative pathway complement regulation is the “defense”, and formation of C3 convertase is the “basket”. Haemolytic uraemic syndrome (HUS) is a triad of thrombocytopenia, MAHA, and acute renal failure. Atypical haemolytic uraemic syndrome (aHUS) has been used broadly to describe any case of HUS that is not caused by shiga toxin‐producing bacteria.
Mechanisms Of Action
- It has to be noted, however, that genetic mutations on complement factors and ADAMTS13 activity were not evaluated in all patients.
- In fact kidney function almost always returns to the normal range within a few months.
- Proteinuria is described as an indirect sign of the anticancer effect of this drug.
- When antibody-mediated TMA is suspected, a trial with plasmapheresis could be useful.
- Other nephrotoxins should be avoided any time close to the conditioning regimen 88, and platelet and RBC transfusion could be indicated 8.
- Recently, there have been some reports of CPIs-induced TMA with ipilimumab and nivolimumab.
Thrombocytopenia, MAHA, and end organ damage are the common elements of all TMAs. MAHA is caused by red blood cell fragmentation in the microvasculature, with schistocytes seen on peripheral blood film. Lactate dehydrogenase (LDH) is raised due to tissue ischemia and cell lysis. Low plasma haptoglobin is a marker of haemolysis as it binds to free haemoglobin and the complex is cleared by macrophages.
COMPLEMENT‐MEDIATED ATYPICAL HAEMOLYTIC URAEMIC SYNDROME
Numerous drugs are described in scientific literature as causative of TMA, mostly as little case series, and the number is rapidly increasing (see Table 1). The drugs reported as causative of TMA are heterogeneous in terms of mechanism of action. Some drugs are more frequently used in clinical activity, as antibiotics or antiplatelet therapy, some others in more restricted contexts, such as IO-anti-VEGF.
In conclusion, the efficacy of eculizumab treatment in DITMA needs to be clarified with further prospective studies, with homogeneous timing of eculizumab infusion and selection of patients with similar clinical and prognostic features. In many of the more atypical TTP/HUS disease patterns the optimal treatment has not yet been standardized. These are often treated (like TTP) with plasma exchange, but there is currently some debate about this. They are generally not controlled or randomized and do not lend themselves to a stricter guideline-based methodology or a Grading of Recommendations Assessment, Development and Evaluation (GRADE)-based approach.
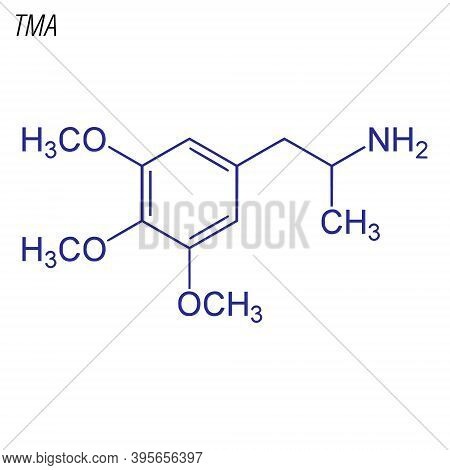
It is characterized by a Coombs-negative microangiopathic haemolytic anemia, thrombocytopenia and organ injury, with characteristic pathological features, resulting from platelet microvascular occlusion. This patient had also taken naproxen and therefore her serum was also tested for naproxen and naproxen glucuronide-dependent, platelet-reactive antibodies. This patient had also taken levaquin and therefore her serum was also tested for levaquin-dependent, platelet-reactive antibodies. Number of patients diagnosed with TA-TMA among total number of patients undergoing hematopoietic cell transplantation. The median follow-up duration varies by study from 100 days to 180 days.